Marwood’s proprietary data module consists of claims-based information assembled over decades and uniquely refined through a consultancy lens to deliver one-of-a-kind, actionable insights that our clients use to transform healthcare companies.
Marwood provides analyses at a national, state and local level to help our clients understand trends in volume and utilization, navigate payor decision-making, and predict future rates and methodology used by Medicare, Medicare Advantage, Medicaid, Medicaid Managed Care, workers’ compensation and commercial insurance payors.
20+ Years
Marwood's unparalleled knowledge of stakeholder strategic needs from 20+ years of advising clients across the industry
12 Billion
Proprietary dataset of nearly 12 billion provider and payor claims across commercial, Medicare, and Medicaid, updated quarterly
Data Team
Marwood's infrastructure, software, and data analytics team is solely dedicated to refining and analyzing data
Marwood Claims Data Insights
See How Marwood Used Our Proprietary Data and Claims Analysis Capabilities to Support a National Dermatology Provider’s Contracting and Growth Strategy …
Marwood Case Study
Engagement Purpose
Marwood was engaged to gather and analyze reimbursement and claims data from a variety of in-house, Client, and third-party datasets in order to derive code-specific benchmarking and determine potential for growth opportunities across potential expansion geographies.
Marwood Analysis
- Evaluated states based on current reimbursement rates and outlook (most heavily weighted), contracting approach for dermatology providers, utilization management (UM) outlook for dermatology, and payor market consolidation
- Created detailed state profiles and summary profiles for 17 states
- Incorporated feedback from executives at 66 plans and third-party commercial claims data to identify which states have the most favorable commercial payor dynamics for a dermatology provider
Key Findings
Marwood applied a blended weighted average to identify reimbursement rates the Company may receive in each state, taking into consideration plan market share, top Company codes, and mid-level versus physician code billing and reimbursement dynamics.
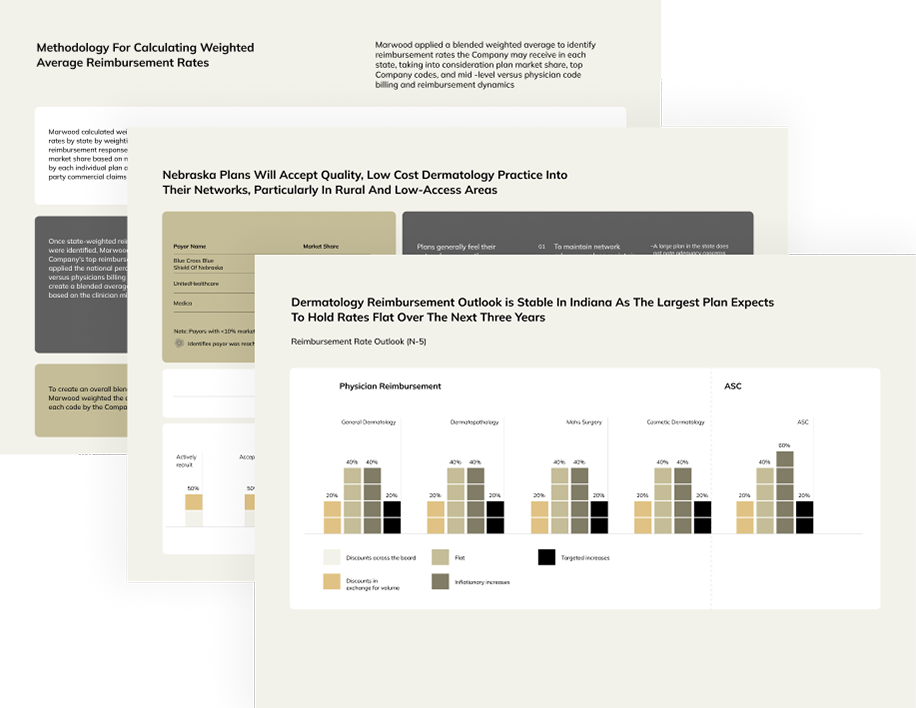
Illustrative example only*
Sign Up for Marwood's Healthcare Newsletter